Radiation generates an abscopal response and complete resolution of metastatic squamous cell carcinoma of the anal canal: a case report
Introduction
The abscopal response is a phenomenon in which radiation therapy (RT) can elicit immune responses that mediate regression of metastatic disease distant from the radiation (1-3). This effect has been observed in a variety of cancer types (4), but has not been described in squamous cell carcinoma of the anus (SCCA). Indeed, only one case of the abscopal effect in squamous cell carcinoma has been reported, involving the uterine cervix (5). The incidence of anal cancer is on the rise, with approximately 27,000 incident cases globally (6,7). Distant metastasis has been observed in 5–8% of cases at initial presentation and in 10–20% of cases after curative local treatment (8). Due to the rarity of metastatic SCCA, evidence-based guidelines defining optimal treatment are lacking, and the first randomized trial is likely not to be reported for many years (9). A common feature of SCCA is the presence of human papilloma virus (HPV) infection, seen in 80–90% of patients with SCCA (10). Viral proteins may be expressed by SCCA and contribute to an immune response (11). The mechanisms behind the abscopal effect are thought to involve induction of a systemic anti-tumor immune response which may be mediated by secretion of effector cytokines, immunogenic cell death and release of neoantigens recognized by the adaptive immune system (2,3,12-14). This report will describe the first case of the abscopal effect in anal cancer and discuss potential implications for clinical research.
Case presentation
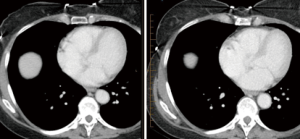
A 57-year-old Caucasian female patient presented with a one-year history of rectal bleeding. Colonoscopy 15 months prior was normal. With increasing bleeding, fatigue, and anal discomfort, she was subsequently referred to a general surgeon in December 2012. Physical examination found a tumor involving the entire anal canal with a protruding perianal component. Tissue diagnosis was obtained by incisional biopsy removing approximately a quarter of the mass. The pathology was poorly differentiated basaloid squamous cell carcinoma with high mitotic activity and strong immunostaining for p16. Staging computerized tomography (CT) scan of the abdomen and pelvis demonstrated thickening involving the right lateral wall of the anal canal, with the cranial margin above the levator muscles. Suspicious lymphadenopathy was identified in the mesorectum and the right internal iliac and obturator nodes. There were several vague low-density foci in both hepatic lobes, the largest measuring 1.3 cm, that were suspicious for metastatic disease (Figures S1,S2).

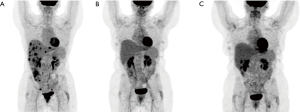
The patient was referred for oncologic assessment and was reviewed in consultation February 2013 by a radiation oncologist and medical oncologist. On digital examination, a mass was noted protruding from the anal orifice, occupying the entire length of the anal canal with at least 1 cm extension into the rectum. Nodular densities were palpable in the rectal submucosa, consistent with mesorectal nodes. Squamous carcinoma antigen was elevated at 4.7 µg/L (normal <1.5). Fluorodeoxyglucose positron emission tomography (FDG PET) scan in February 2013 (Figure 1A) confirmed malignant involvement of the anal canal with multiple perirectal and right internal iliac lymph node metastases. Approximately 16 hepatic metastases were identified, the largest measuring 2.8 cm with a maximum standardized uptake value (SUVmax) of 9.4. There was an FDG avid lesion measuring 1.6 cm in the right iliac bone consistent with bone metastasis.
After multidisciplinary review, the patient was offered high dose palliative radiation to the pelvis with concurrent chemotherapy as a radiation sensitizer, with the aim of providing long-term symptom control. Using CT-based 3-D conformal planning, RT encompassed the primary anal tumour, affected pelvic lymph nodes, and iliac bone metastasis. A total dose of 54 Gy in 30 fractions (1.8 Gy/fraction) was delivered to the primary tumor, and 50.4 Gy to the nodal and bone metastases. The liver was not treated with RT. Chemotherapy consisted of capecitabine 750 mg/m2 twice daily on each day of RT, and Mitomycin C 10 mg/m2 on days 1 and 28. All treatment was completed in April 2013 with minimal toxicity.
Four weeks after RT completion, CT of the abdomen and pelvis demonstrated regression of the multiple liver metastases, with a solitary 5 mm lesion remaining visible (Figures S1,S2). At 5 weeks, squamous carcinoma antigen decreased to 1.5 µg/L. Clinical examination at 6 weeks found the anal tumour and perirectal nodularity to be completely resolved. As the primary and metastatic disease regressed and the patient was no longer symptomatic, no further treatment was recommended.
Follow-up assessment including history, physical examination, and CT scans at 4, 7, and 10 months post therapy, and subsequently every 6–12 months found no evidence of disease. In January 2016, a transient rise in squamous carcinoma antigen to 2.5 µg/L was observed. This was evaluated with PET imaging February 2016 demonstrating no evidence of disease (Figure 1B). The squamous carcinoma antigen subsequently returned to normal levels without intervention. On the last follow-up visit in February 2017, there were no symptoms or signs of recurrent disease. PET scan in March 2017, 4 years after treatment, shows no evidence of disease (Figure 1C).
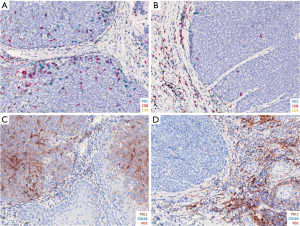
After the patient provided written informed consent for retrieval of tumor tissue blocks, automated multi-parametric immunostaining was performed to evaluate immune markers of tumor infiltrating lymphocytes (TILs) including programmed cell death 1 (PD1; clone NAT105), programmed cell death ligand 1 (PDL1; clone SP142), CD163 (macrophages; clone 0D6), CD3 and CD8 (T cells; clone SP7 & C8/144B) (15,16). Staining with immune markers showed a significant degree of tumor heterogeneity. Some regions of tumor were densely infiltrated with lymphocytes, including CD8+ and CD4+ T cells (Figure 2A), suggesting a propensity towards an exuberant immune response. Other regions displayed lymphocyte staining predominantly at the boundary between the stroma and epithelium (Figure 2B). In contrast to T cells found in the stroma, a larger portion of intratumor TILs co-expressed PD1. Expression of PDL1 was also observed in the tumor (Figure 2C) and stromal macrophages (Figure 2D), suggesting inhibition at the immune checkpoint level.
Discussion
Treatment for patients with metastatic SCCA is not well defined (8). Depending on symptoms and location of disease, options may include chemotherapy and palliative RT (8). Available data are limited to retrospective studies with small samples reporting short median survival of 8–12 months (7). Patients presenting with small volume distant disease may be eligible for aggressive local treatment of the metastatic lesions, with a median progression free survival of 16 months, compared to 5 months with palliative chemotherapy alone (7). The current case, presenting with multiple liver metastases, treated with pelvic RT and radiosensitizing chemotherapy resulting in long-term complete remission is unique. We hypothesize that the local pelvic RT provoked an abscopal immune response resulting in complete resolution of the liver metastases.
Alternative potential explanations of the dramatic response in the liver include other disease entities or an exquisitely sensitive metastatic anal cancer that responded fully to the radiosensitizing chemotherapy. As the staging PET findings were consistent with multiple metastatic liver lesions, an invasive procedure to obtain tissue diagnosis of the liver was not pursued. After the unexpected complete response was observed, we retrospectively obtained independent review by a radiologist with expertise in functional imaging to address the question of whether the hepatic lesions may represent non-malignant disease such as a benign inflammatory condition. The PET and CT review, which took into consideration the number and distribution of the liver lesions and their SUV characteristics, deemed that metastatic anal cancer remained the most likely diagnosis. Perhaps a second malignancy such as an occult breast carcinoma that responded fully to the capecitabine and mitomycin could be responsible. However, the patient had a normal mammogram and the PET scan found no evidence of other primary malignancy.
The possibility that the hepatic lesions were metastatic anal carcinoma that responded completely to capecitabine and mitomycin at radiosensitizing doses was also considered. However, a United Kingdom randomized trial of chemoradiotherapy for localized disease used a comparable regimen of 5-fluorouracil (5-FU) and mitomycin plus RT failed to demonstrate a reduction in distant metastasis compared to RT alone (17), suggesting the chemotherapy regimen used in our case was highly unlikely to produce a complete response in the overt metastatic disease. In addition, studies of palliative chemotherapy regimens with dose-intense schedules have reported response rates of approximately 50%, with complete response rates in the range of 6–20% (7,18,19). Typical palliative chemotherapy regimens for metastatic SCCA are cisplatin and 5-FU, or carboplatin and paclitaxel (7,8). In a retrospective study of 77 patients with metastatic SCCA, the median progression free survival and overall survival were 7 and 22 months respectively with chemotherapy alone (7). Our literature search identified only a single report describing complete, prolonged response to palliative chemotherapy in a patient who received six cycles of cisplatin and 5-FU and was cancer-free for seven years after treatment (20).
Local pelvic RT triggering an abscopal immune response resulting in complete regression of the liver metastases is a strong consideration in this case. The dense infiltration of lymphocytes observed within the tumor and the stroma suggests a strong immune response in this patient’s disease. That the tumor cells stained strongly for PDL1 suggests that immune checkpoint inhibition was keeping the host response at bay. The mechanisms responsible for this response may have included an attenuation of the immune checkpoint inhibition through downregulation of PDL1 expression, as well as presentation of viral neoantigens. Although it would have been interesting to have biopsy samples from the metastatic liver lesions before and after pelvic RT, it was not possible to have recognized beforehand that this patient was going to have a dramatic metastatic response.
While the mechanisms behind the abscopal effect are not entirely understood, many hypotheses have been explored. It is generally thought that local RT enhances the ability of the immune system to recognize and respond to a distant cancer (3,14), as though the tumor were induced to become an in-situ vaccine against itself and its related metastases. In addition to spatial anti-tumor effects, temporal immune effects might prevent proliferation of clones emerging from a dormant state. Various mechanisms have been proposed, including alterations of antigen presentation, T-cell activation, cytokine release and alteration in checkpoint inhibition (2,3,10,11,21-24). As the majority of SCCA are related to HPV infection, it is tempting to speculate that viral oncoproteins expressed by the tumor may act as antigens for immunotherapies (10).
A promising avenue to explore in SCCA treatment is the role of immune checkpoint inhibitors, the expression of which may allow cancer to evade immune detection. Checkpoint inhibitors such as cytotoxic T lymphocyte associated antigen 4 (CTLA-4), PD1, and PDL1 may be overexpressed in cancer cells as was seen in this case. Local RT has been reported to decrease the expression of PDL1 thereby modulating the immune inhibition (25). In a retrospective study, Morris et al. reported that 56% of 41 patients with SCCA had PDL1-positive disease (10). A phase II trial of nivolumab, an anti-PD1 antibody which prevents the interaction between PD1 and its ligand PDL1, disrupting the inhibited T-cell immune response, enrolled patients with metastatic SCCA refractory to palliative chemotherapy. Of 37 trial participants, two had complete response and seven had partial response (11).
Interestingly, most of the research on the potentiation of the immune system has focused on hypofractionated RT employing large doses of >2 Gy per fraction (25). While some investigators have suggested that hypofractionation is associated with a stronger immune response (26), others have reported that conventional RT fractionation with 1.8–2 Gy per fraction such as that used in the current case, is associated with higher levels of interactions with the immune system (27). Research evaluating the interactions between different RT regimens and immune potentiation is thus needed.
Conclusions
The case described contributes the first report of the abscopal effect in squamous cell cancer of the anal canal. The observations in this case suggest that the abscopal phenomenon represents an exciting avenue of research that may improve insight into the interactions between RT and the immune response and may lead to the development of new therapeutic strategies that utilize the synergies of these two modalities. Metastatic SCCA may be a promising clinical model for such studies due to its association with viral oncoprotein expression. For patients with metastatic SCCA, an orphan disease with limited treatment options, trials to evaluate the effect of immune checkpoint inhibitors and RT to provoke heightened abscopal response are warranted.
Acknowledgements
We thank the subject of this case report for providing written informed consent and the Molecular Cancer Immunology Core for help with staining samples.
This work was supported by funds from the Canadian Institute of Health Research (JJ Lum).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and all accompanying images.
References
- Mole RH. Whole body irradiation—radiobiology or medicine? Br J Radiol 1953;26:234-41. [Crossref] [PubMed]
- Demaria S, Ng B, Devitt M, et al. Ionizing radiation inhibition of distant untreated tumors (abscopal effect) is immune mediated. Int J Radiat Oncol Biol Phys 2004;58:862-70. [Crossref] [PubMed]
- Reynders K, Illidge T, Siva S, et al. The abscopal effect of local radiotherapy: using immunotherapy to make a rare event clinically relevant. Cancer Treat Rev 2015;41:503-10. [Crossref] [PubMed]
- Abuodeh Y, Venkat P, Kim S. Systematic review of case reports on the abscopal effect. Curr Probl Cancer 2016;40:25-37. [Crossref] [PubMed]
- Takaya M, Niibe Y, Tsunoda S, et al. Abscopal effect of radiation on toruliform para-aortic lymph node metastases of advanced uterine cervical carcinoma - a case report. Anticancer Res 2007;27:499-503. [PubMed]
- de Martel C, Ferlay J, Franceschi S, et al. Global burden of cancers attributable to infections in 2008: a review and synthetic analysis. Lancet Oncol 2012;13:607-15. [Crossref] [PubMed]
- Eng C, Chang G, You Y, et al. The role of systemic chemotherapy and multidisciplinary management in improving the overall survival of patients with metastatic squamous cell carcinoma of the anal canal. Oncotarget 2014;5:11133. [Crossref] [PubMed]
- Glynne-Jones R, Nilsson P, Aschele C, et al. Anal cancer: ESMO–ESSO–ESTRO clinical practice guidelines for diagnosis, treatment and follow-up. Radiother Oncol 2014;111:330-9. [Crossref] [PubMed]
- InterAACT trial. Available online: https://clinicaltrials.gov/show/NCT02051868
- Morris VK, Rashid A, Rodriguez-Bigas M, et al. Clinicopathologic features associated with human papillomavirus/p16 in patients with metastatic squamous cell carcinoma of the anal canal. Oncologist 2015;20:1247-52. [Crossref] [PubMed]
- Ndiaye C, Mena M, Alemany L, et al. HPV DNA, E6/E7 mRNA, and p16 INK4a detection in head and neck cancers: a systematic review and meta-analysis. Lancet Oncol 2014;15:1319-31. [Crossref] [PubMed]
- Morris V, Eng C. Summary of emerging targets in anal cancer: the case for an immunotherapy based-approach. J Gastrointest Oncol 2016;7:721-6. [Crossref] [PubMed]
- Morris VK, Salem ME, Nimeiri H, et al. Nivolumab for previously treated unresectable metastatic anal cancer (NCI9673): a multicentre, single-arm, phase 2 study. Lancet Oncol 2017;18:446-53. [Crossref] [PubMed]
- Siva S, MacManus M, Martin R, et al. Abscopal effects of radiation therapy: a clinical review for the radiobiologist. Cancer Lett 2015;356:82-90. [Crossref] [PubMed]
- Webb JR, Milne K, Kroeger DR, et al. PD-L1 expression is associated with tumor-infiltrating T cells and favorable prognosis in high-grade serous ovarian cancer. Gynecol Oncol 2016;141:293-302. [Crossref] [PubMed]
- Kroeger DR, Milne K, Nelson BH. Tumor-infiltrating plasma cells are associated with tertiary lymphoid structures, cytolytic T-cell responses, and superior prognosis in ovarian cancer. Clin Cancer Res 2016;22:3005-15. [Crossref] [PubMed]
- Northover J, Glynne-Jones R, Sebag-Montefiore D, et al. Chemoradiation for the treatment of epidermoid anal cancer: 13-year follow-up of the first randomised UKCCCR Anal Cancer Trial (ACT I). Br J Cancer 2010;102:1123-8. [Crossref] [PubMed]
- Faivre C, Rougier P, Ducreux M, et al. 5-fluorouracil and cisplatinum combination chemotherapy for metastatic squamous cell anal cancer. Bull Cancer 1999;86:861-5. [PubMed]
- Kim R, Byer J, Fulp W, et al. Carboplatin and paclitaxel treatment is effective in advanced anal cancer. Oncology 2014;87:125-32. [Crossref] [PubMed]
- Haydon A, Tay R, Mak G, et al. Long survival (cure) to cisplatin/infusional 5-fluorouracil in metastatic squamous cell anal cancer with extensive liver and lung metastases. Case Reports in Clinical Medicine 2015;4:73-6. [Crossref]
- Geng Y, Shao Y, He W, et al. Prognostic role of tumor-infiltrating lymphocytes in lung cancer: a meta-analysis. Cell Physiol Biochem 2015;37:1560-71. [Crossref] [PubMed]
- Kotera Y, Shimizu K, Mulé JJ. Comparative analysis of necrotic and apoptotic tumor cells as a source of antigen(s) in dendritic cell-based immunization. Cancer Res 2001;61:8105-9. [PubMed]
- Tinhofer I, Budach V, Jöhrens K, et al. The rationale for including immune checkpoint inhibition into multimodal primary treatment concepts of head and neck cancer. Cancers of the Head & Neck 2016;1:8. [Crossref]
- Reits EA, Hodge JW, Herberts CA, et al. Radiation modulates the peptide repertoire, enhances MHC class I expression, and induces successful antitumor immunotherapy. J Exp Med 2006;203:1259-71. [Crossref] [PubMed]
- Bernstein MB, Krishnan S, Hodge JW, et al. Immunotherapy and stereotactic ablative radiotherapy (ISABR): a curative approach? Nat Rev Clin Oncol 2016;13:516-24. [Crossref] [PubMed]
- Schaue D, Ratikan J, Iwamoto K, et al. Maximizing tumor immunity with fractionated radiation. Int J Radiat Oncol Biol Phys 2012;83:1306-10. [Crossref] [PubMed]
- Rubner Y, Muth C, Strand A, et al. Fractionated radiotherapy is the main stimulus for the induction of cell death and of Hsp70 release of p53 mutated glioblastoma cell lines. Radiat Oncol 2014;9:89. [Crossref] [PubMed]
- Joe MB, Lum JJ, Watson PH, et al. CT images showing multiple liver metastases pre-treatment on left hand panel and resolution of liver disease on right hand panel 4 weeks after pelvic radiation therapy and chemotherapy. Asvide 2017;4:514. Available online: http://www.asvide.com/articles/1833